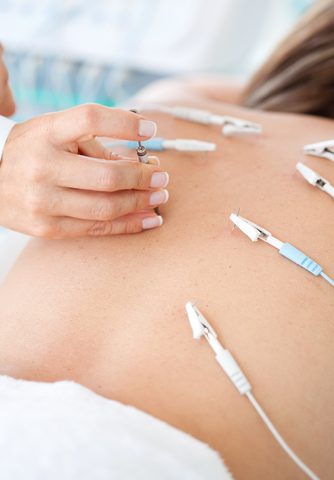
A new protocol designed to maximize the intensity of the electrical stimulus used in transcutaneous electrical nerve stimulation (TENS) may benefit older and more anxious patients with fibromyalgia.
These findings were reported in the study “Development of a method to maximize the transcutaneous electrical nerve stimulation intensity in women with fibromyalgia” that appeared in the Journal of Pain Research.
TENS is a non-pharmacological, non-invasive therapy that has been proposed to treat patients who have chronic pain, including fibromyalgia. It uses electrical pulses to activate the opioid system in the peripheral and central nervous systems and alter the sensation of pain.
Clinical trials have shown that TENS can reduce pain and the amount of pain medication needed, as well as improve function of patients with acute or chronic pain conditions.
Although the effects of this alternative therapeutic method are still controversial, cumulative evidence suggests that the effectiveness of TENS depends mostly on the electrical frequency applied.
While higher frequencies seem to be more efficient to manage pain, achieving the adequate TENS intensity can be a challenge as it is related to each patient’s pain severity, disease severity, or psychological variables.
A team led by researchers at the University of Iowa looked at whether exposure to the full range of clinical levels of electrical stimulation — from sensory threshold to noxious — would result in higher final stimulation intensities.
The study (NCT01888640) included 143 women with diagnosed fibromyalgia and moderate symptoms, as determined by the Revised Fibromyalgia Impact Questionnaire (FIQR) score, who underwent TENS applied to the lumbar area.
The new Setting of Intensity of TENS (SIT) test protocol began with a baseline intensity identified as sensory threshold, which was then increased to “strong but comfortable” (SC1) and then to “noxious” (N). This was followed by a reduction to the final stimulation intensity of “strong but comfortable” (SC2).
The median TENS intensity achieved was 37.5 mA for SC1, 40.4 mA for N, and 39.2 mA for SC2. mA is a measure of intensity.
Patients had a range of responses to the differences between SC1 and SC2 attained values, with 30.1% having an increase of at least 5 mA and 12.6% having an increase of at least 10 mA.
Despite several analyses, the researchers could not find significant correlations between the intensities of SC1, SC2, and N and patient characteristics, including age, weight, pain scores, symptom severity scores, depression and anxiety scores, or pain catastrophizing scale scores.
Still, the patients’ pattern of response varied among groups based on age and anxiety scores. Patients older than 40 years and those with higher anxiety levels were able to achieve greater increases in intensity (SC2–SC1) after a trial of noxious stimulation intensity.
These results suggest that “pain and its related symptoms do not directly influence the precise level of TENS stimulation intensity,” researchers said. Still, the SIT protocol seems to promote greater intensity changes in older women and women with elevated anxiety.
“It is unclear, however, what factors will be predictors of TENS effectiveness in women with fibromyalgia, or if the ability to achieve the greatest change in intensity between SC1 and SC2 is related to TENS effectiveness,” they wrote.
Completion of the analysis of the trial data is expected to provide valuable information on the effectiveness and utility of the SIT test.