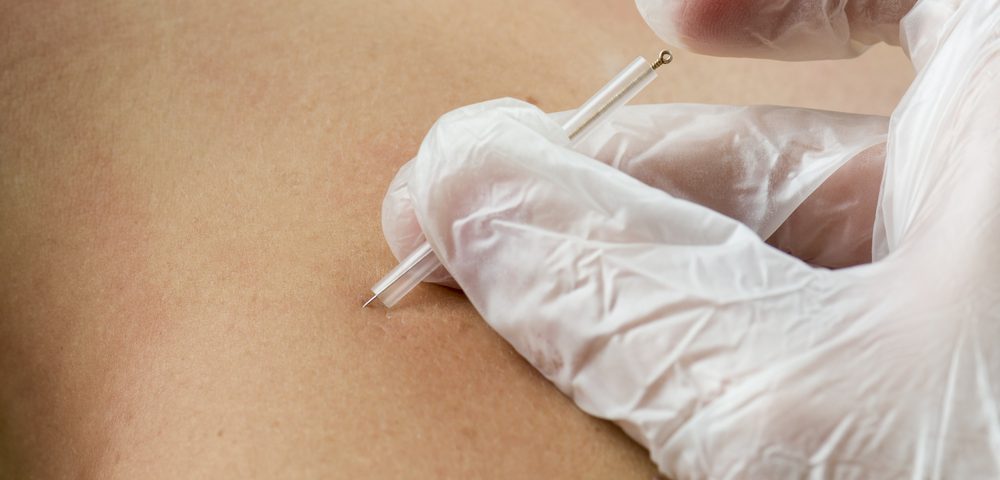
A treatment for fibromyalgia known as dry needling reduces pain stemming from trigger points and increases spinal mobility, according to a clinical study.
The technique uses needles to affect sensitive points in the muscle, which cause pain in seemingly unrelated body parts. Inactivating these trigger points appears to decrease pain.
The study, “Effects of Dry Needling on Spinal Mobility and Trigger Points in Patients with Fibromyalgia Syndrome,” was published in Pain Physician Journal and reported the results of a clinical trial (NCT02380807).
In the study, the effects of dry needling in the spinal muscles (thoracic and lumbar) of fibromyalgia patients were compared to cross taping, which uses a nonelastic cross-mesh tape applied to the same trigger points.
Patients were recruited at the Virgen de la Arrixaca University Hospital in Murcia, Spain. A total of 64 patients were randomly placed in either dry needling or cross-tape therapy groups. All participants received a baseline test, followed by four once-weekly therapy sessions. Five men and 59 women, whose ages ranged from 27 to 58, participated in the study.
Trigger points included broad back muscle or “lats” (latissimus dorsi), extensor back muscles (iliocostalis, multifidus), and quadratus lumborum muscles, which, although located in the lower back, are actually the deepest abdominal muscle. Spinal mobility and pain measurements were recorded at baseline and after five weeks of treatment.
The results showed a significant difference between the two groups.
“In this study, a 4-week dry-needling therapy significantly decreased the number of MTrPs [myofascial trigger points] in comparison to the cross-tape group, mainly in MTrPs of the latissimus dorsi, multifidus, and quadratus lumbourum muscles. Dry needling also showed a major improvement in pain intensity,” the researchers wrote in their report.
“Dry needling and cross tape approaches reported a similar effect size for spinal mobility measures, with the exception of the dry needling group in a sitting position, where dry needling showed a major improvement,” the team reported.
The scientists, however, acknowledged three main limitations in the study: “The outcomes were not collected from a long-term follow-up period. Dry needling therapy or cross tape were used alone when in reality physical therapists usually treat patients with [fibromyalgia] using a multi-modal approach. A non-treatment control group was not included.”
Therefore, the team suggests that future investigations are needed to determine the long-term effectiveness of the technique in fibromyalgia patients.