The Toronto General Hospital’s Transitional Pain Service has chosen ManagingLife’s ‘Manage My Pain’ mobile app to help prevent chronic post-surgical pain in at-risk patients. The cloud-based smartphone app, claiming to have more than 20,000 users in over 130 countries, enables chronic pain sufferers with conditions like fibromyalgia, back pain, and migraines to digitally and regularly record a journal in which they describe and track the pain they’re experiencing and share those descriptions with their physicians.
ManagingLife — a private corporation based in Toronto, Canada, that develops mobile tools to connect patients and clinicians for more efficient and effective pain management — says chronic postsurgical pain (CPSP) develops in 5 percent to 10 percent of patients within one year after major surgery, and is estimated to have direct and indirect costs of U.S. $41,000 per patient. Additionally, CPSP takes a devastating toll, with consequences that may include depression, disability, and opioid dependency or abuse.
Toronto General Hospital, part of the University of Toronto Health Network in Toronto, Ontario, is Canada’s leading surgical center with more than 6,000 surgeries performed annually. The Transitional Pain Service (TPS) is one of the world’s first programs to proactively and comprehensively address the problem of Chronic Postsurgical Pain (CPSP) for at-risk patients. Through coordinated care by a multidisciplinary team of therapists consisting of pain physicians, advanced practice nurses, psychologists, and physiotherapists, TPS begins before a patient undergoes surgery and continues for up to six months after the patient is discharged.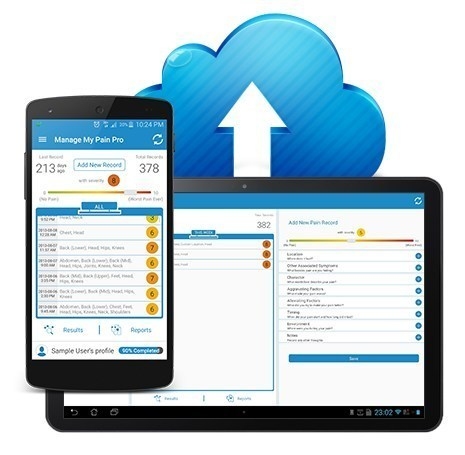
The TPS is profiled in an article recently published in the Journal of Pain Research, entitled “The Toronto General Hospital Transitional Pain Service: development and implementation of a multidisciplinary program to prevent chronic post surgical pain” (J Pain Res. 2015 Oct 12;8:695-702. doi: 10.2147/JPR.S91924. eCollection 2015). It is co-authored by Joel Katz, Aliza Weinrib, Samantha R Fashler, Rita Katznelzon, Bansi R. Shah, Salima S.J. Ladak, Jiao Jiang, Qing Li, Kayla McMillan, Daniel Santa Mina, Kirsten Wentlandt, Karen McRae, Diana Tamir, Sheldon Lyn, Marc de Perrot, Vivek Rao, David Grant, Graham Roche-Nagle, Sean P. Cleary, Stefan O.P. Hofer, Ralph Gilbert, Duminda Wijeysundera, Paul Ritvo, Tahir Janmohamed, Gerald O’Leary, and Hance Clarke, variously representing the Toronto General Hospital Department of Anesthesia and Pain Management and Department of Anesthesia at the University of Toronto; the York University Department of Psychology in Toronto; the Princess Margaret Cancer Centre, Faculty of Kinesiology and Physical Education, Palliative Care program, and Department of Family and Community Medicine; the Toronto General Hospital, York University Divisions of Thoracic Surgery and Cardiovascular Surgery, Multiorgan Transplant Program, Division of Vascular Surgery, Division of General Surgery, Division of Plastic Surgery, Division of Otolaryngology – Head and Neck Surgery, and Department of Kinesiology and Health Science, York University; and ManagingLife of Toronto, Ontario, Canada.
The co-authors note that substantial advances have been made in identifying patients at elevated risk of developing CPSP based on perioperative pain, opioid use, and negative affect, which can include depression, anxiety, pain catastrophizing, and post-traumatic stress disorder (PTSD)-like symptoms, and that The Toronto General Hospital Transitional Pain Service is the first to comprehensively address the problem of CPSP at three stages: 1) preoperatively, 2) postoperatively in hospital, and 3) postoperatively in an outpatient setting for up to six months.
The Journal of Pain Research article explains that after patients at high risk for CPSP are identified, they are offered coordinated and comprehensive care by the multidisciplinary team, bypassing typically long waits to be referred and seen in chronic pain clinics. This timely access to therapy enables the clinicians to impact patients’ pain trajectories, preventing the transition from acute to chronic pain, and reducing suffering, disability, and healthcare costs.
In the report, the co-authors describe the workings of the TPS at Toronto General, including the clinical algorithm used to identify patients, and the clinical services offered as patients transition through the stages of surgical recovery. They describe the role of psychological treatment, which draws on innovations in Acceptance and Commitment Therapy that allow for brief and effective behavioral interventions to be applied transdiagnostically and preventively. Finally, they describe a vision for future growth.
Calling chronic pain the silent epidemic of our time, the investigators estimate the economic costs of chronic pain in the U.S. to now exceed that of heart disease, cancer and diabetes, and that chronic postsurgical pain is a significant driver of those costs ($41,000 per patient). Given that the one-year incidence of moderate-to-severe CPSP is between 5 percent and 10 percent, and that worldwide, more than 230 million people undergo major surgery every year, the global annual cost of new CPSP cases is likely in the hundreds of billions of dollars.
Equally troubling, they observe, is the humanitarian cost of CPSP — too frequently the unanticipated result of necessary and even life-saving surgery, depriving the individual of vital energy and productivity, and leading to many negative secondary, downstream effects.
The co-authors note that response to this costly tragedy has been unacceptably slow, and that while for more than 20 years the center have been making progress in managing acute post-surgical pain through new insights and novel findings in pre-emptive/preventive analgesia, comparable breakthroughs have not been made in minimizing the transition to CPSP.
Accordingly, they recommend adopting a multidisciplinary preventive approach involving intensive, perioperative psychological, medical, physical therapy, and pharmacological management interventions focused on preventing and treating the factors that increase the risk of CPSP and associated disability.
In the paper, the co-authors briefly review the main risk factors for CPSP and then describe the Transitional Pain Service (TPS) which they have developed and implemented since 2014: identify patients at risk of CPSP; intervene in a tailored and timely way medically and psychologically; and reduce reliance on opioid medications by focusing on treatment across the hospital-to-home trajectory. The researchers anticipate that the TPS will produce substantial savings, shorter hospital stays, earlier weaning from opioid analgesic medications, reduced emotional distress, improved quality of life, and reduced incidence and severity of CPSP and disability. They note that preliminary data already support some of these anticipated outcomes, and that data from their and other published literature clearly show the following factors predict CPSP risk across a range of surgical procedures:
• perioperative pain (the presence and intensity of preoperative pain, high intensity acute postoperative pain),
• perioperative opioid use
• preoperative negative affective states including PTSD-like symptoms
• depression
• anxiety
• pain catastrophizing
The known psychological risk factors for CPSP (negative affect, catastrophizing) are also risk factors for intense, acute postoperative pain and high/excessive use of opioid analgesics in the acute postoperative setting. Inadequately controlled acute pain and excessive analgesic use have been repeatedly shown to delay recovery and hospital discharge. The researchers’ own data show that 3 percent of previously opioid-nave patients continue to use opioids 90 days after major elective surgery, and explain that the TPS is designed to target and manage these known risks pre- and postsurgery.
The mission of the TPS is to treat patients at risk of transitioning from acute to CPSP. As such, it is the first service to comprehensively address the problem of CPSP after major surgery through multidisciplinary, coordinated care beginning preoperatively, extending postoperatively, and continuing once patients have returned home.
The co-authors say the three primary goals of the TPS are to:
1) provide a novel, seamless approach to pre- and postoperative pain management for patients who are at increased risk for developing CPSP and pain disability,
2) manage opioid medication for medically complex patients post-discharge,
3) improve patient coping and functioning to ensure as high a quality of life as possible after surgery.
The researchers conclude that current TPS and planned expansions are designed to address the historical gaps in pain management for postsurgical patients, and their goals include evaluating the extent to which the TPS reduces hospital stay, hospital readmission rates, and overall costs to the healthcare system.
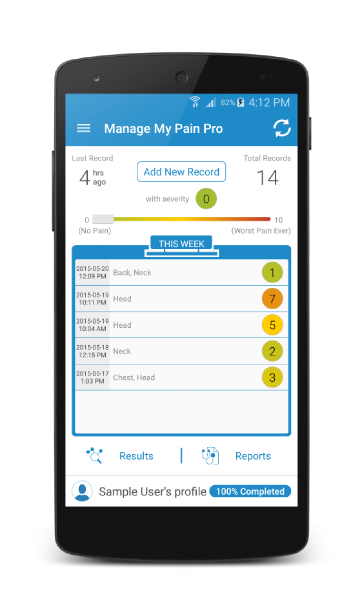 Essential to TPS effectiveness is the ability to engage, monitor, and intervene with patients in the critical months following surgery. TPS patients will use the Manage My Pain app to record their pain once discharged from hospital, with data collected remotely being monitored by the TPS team.
Essential to TPS effectiveness is the ability to engage, monitor, and intervene with patients in the critical months following surgery. TPS patients will use the Manage My Pain app to record their pain once discharged from hospital, with data collected remotely being monitored by the TPS team.
In an Open Forum blog entitled “Changing the way chronic pain is managed,” ManagingLife CEO Tahir Janmohamed, also a journal co-author, notes that the app helps people track, analyze, and share their
pain to help them better understand their conditions and communicate with their doctors and insurance companies. He adds that the app’s easy-to-use interface and doctor-friendly reports have allowed it to become one of the most downloaded and market-leading pain management apps on Android. With its growing user-base, ManagingLife continues to build one of the largest repositories of self-reported pain information. You can learn more about the app at:
http://www.managinglife.com
Mr. Janmohamed says the app helps bridge breakdowns in patient/doctor communication by providing a common language for both pain sufferer and doctor, taking the traditional paper-based diary and putting it on a smartphone so as to make it easier for pain sufferers to create a record, and enabling valuable insights and analytics.
The app also has detailed reporting and analytics capabilities, enabling evidence-based diagnosis and treatment, and supporting the medical insurance and disability claim process.
“This app will allow patients to stay on top of their pain and medication use on an hourly to daily basis, and enable us to quickly identify patients that are in distress,” says Dr. Hance Clarke, Director of the TPS. “We are hoping that this feedback from our patients outside of the clinic will help us intervene when needed while empowering patients.”
The 18-month demonstration project is funded through Ontario Centres of Excellence’s AdvancingHealth program. The Toronto General Hospital, ManagingLife, and York University partnered for the grant, which is only one of five awarded to healthcare innovators. The project is set to begin in December 2015.
“The AdvancingHealth program helped both us and our partners navigate through some of the challenges of getting impactful innovation into the hospital,” says ManagingLife’s Mr. Janmohamed. “Because of this program, we now have the opportunity to be one of the world’s first quantifiable examples of using mobile health technology to help prevent CPSP and its associated costs.”
For more information, visit:
http://www.managinglife.com/
Note that the Manage My Pain app only suports Android devices.
Sources:
ManagingLife
The Toronto General Hospital
Journal of Pain Research
Open Forum
